Starting on Exemptia
What should I tell my doctor BEFORE starting Exemptia?
Tell your doctor about all of your health conditions, whether you:
- Have an infection, are being treated for infection, or have symptoms of an infection
- Get a lot of infections or infections that keep coming back
- Have diabetes
- Have TB or have been in close contact with someone with TB, or were born in, lived in, or travelled where there is more risk for getting TB
- Live or have lived in an area where there is an increased risk for getting certain kinds of fungal infections, such as histoplasmosis, coccidioidomycosis, or blastomycosis
- Have or have had hepatitis B
- Are scheduled for major surgery
- Have or have had cancer
- Have numbness or tingling (lack of sensation) or a nervous system disease such as multiple sclerosis or Guillain-Barré syndrome
- Have or had heart failure
- Have recently received or are scheduled to receive a vaccine. Exemptia (adalimumab) patients may receive vaccines, except for live vaccines
- Are allergic to any of the Exemptia (adalimumab) ingredients
- Are pregnant, planning to become pregnant, breastfeeding or planning to breastfeed
Also tell your doctor about all the medicines you take. You should not take Exemptia (adalimumab) with abatacept, anakinra, infliximab, etanercept, certolizumab pegol or golimumab. Tell your doctor if you have ever used rituximab, azathioprine or mercaptopurine (6-MP).
What should I watch for AFTER starting Exemptia?
Exemptia can cause serious side effects, including:
- Serious infections. These include TB and infections caused by viruses, fungi, or bacteria. Symptoms related to TB include a cough, low-grade fever, weight loss, or loss of body fat and muscle.
- Hepatitis B infection in carriers of the virus. Symptoms include muscle aches, feeling very tired, dark urine, skin or eyes that look yellow, little or no appetite, vomiting, clay-colored bowel movements, fever, chills, stomach discomfort, and skin rash.
- Allergic reactions. Symptoms of serious allergic reactions include hives (urticaria), trouble during breathing, and swelling of your face, eyes, lips, or mouth.
- Nervous system problems. Signs and symptoms include numbness or tingling, problems with your vision, weakness in your arms or legs, and dizziness.
- Blood problems. Symptoms include a fever that does not go away, bruising or bleeding very easily, or looking very pale.
- Heart failure (new or worsening). Symptoms include shortness of breath, swelling of your ankles or feet, and sudden weight gain.
- Immune reactions including a lupus-like syndrome. Symptoms include chest discomfort or pain that does not go away, shortness of breath, joint pain, or rash on your cheeks or arms that gets worse in the sun.
- Liver problems. Symptoms include feeling very tired, skin or eyes that look yellow, poor appetite or vomiting, and pain on the right side of your stomach (abdomen).
- Psoriasis (new or worsening). Symptoms include red scaly patches or raised bumps that are filled with pus.Call your doctor or get medical care immediately if you develop any of the above mentioned symptoms.Common side effects of adalimumab include injection site reactions (redness, rash, swelling, itching, or bruising), upper respiratory infections (sinus infections), headache, rash, and nausea.These are not all of the possible side effects with Exemptia (adalimumab). Tell your doctor if you have any side effect that bothers you or that does not go away.
Remember, tell your doctor immediately if you have an infection or symptoms of an infection, including:
- Fever, sweats, or chills
- Muscle aches
- Cough
- Shortness of breath
- Blood in phlegm
- Weight loss
- Warm, red, or painful skin or sores on your body
- Diarrhea or stomach pain
- Burning when you urinate
- Urinating more often than normal
- Feeling very tired
Exemptia is given by injection under the skin.
How to administer?
Do not try to inject Exemptia (adalimumab) yourself until you have been shown the right way to give the injections and have read and understood this Instructions for Use. If your doctor decides that you or a caregiver may be able to give your injections of Exemptia at home, you should receive training on the right way to prepare and inject Exemptia (adalimumab). It is important that you read, understand, and follow these instructions so that you inject Exemptia (adalimumab) the right way.
Gather the material required for your injection:
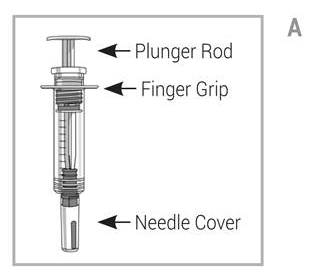
- Alcohol swab
- Cotton ball or gauze pad (not included in your Exemptia carton)
- Exemptia prefilled syringe. See Figure A.
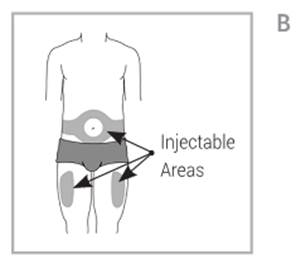
Choose the injection site: wash and dry your hands well. Choose an injection site on:
- The front of your thighs or
- Your lower abdomen (belly). If you choose your abdomen do not use the area 2 inches around your bellu button (navel). See Figure B
- Choose a different site each time you give yourself an injection. Each new injection should be given at least one inch from a site you used before.
- Do not inject into the skin that is:
- Sore (tender)
- bruised
- red
- hard
- scarred or where you have stretch marks
- If you have psoriasis, do not inject directly into any raised, thick, red or scaly skin patches or lesions on your skin.
- Do not inject through your clothes.
Prepare the injection site:
- Wipe the injection site with an alcohol swab using a circular motion.
- Do not touch this area again before giving the injection. Allow skin to dry before injecting. Do not fan or blow on the clean area.
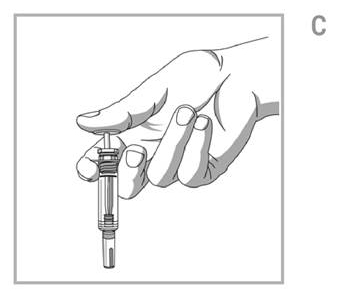
Prepare the syringe and needle:
- Always hold the prefilled syringe by the body of the syringe. Hold the syringe with covered needle pointing down. See Figure C.
- Hold the syringe at eye level
- The top of the liquid may be curved
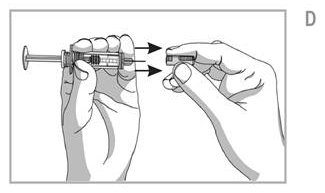
- Remove the needle cover
- Hold the syringe in one hand. With the other hand gently remove the needle cover. See Figure D.
- Throw away the needle cover.
- Do not touch the needle with your fingers or do not let the needle touch anything.
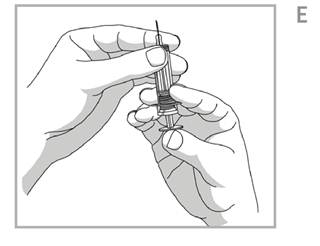
- Turn the syringe so that needle is facing up and hold the syringe at eye level with one hand so you can see the air in the syringe. Using your other hand, slowly push the plunger in, to push the air out throughout the needle. See Figure E.
- You may see a drop of liquid at the end of the needle. This is normal.
Position the prefilled syringe and inject Exemptia:
Position the syringe:
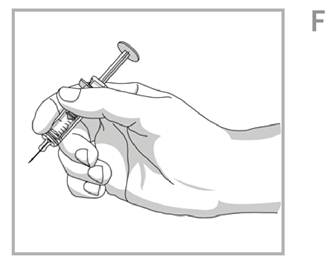
- Hold the body of the prefilled syringe in one hand between the thumb and index finger. Hold the syringe in your hand like a pencil. See Figure F.
- Do not pull back on the plunger at any time.
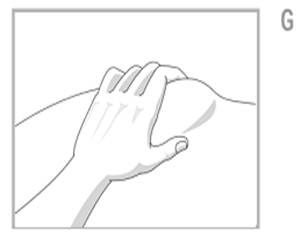
- With our other hand gently squeeze the area of cleaned skin and hold it firmly. See Figure G.
Inject Exemptia:
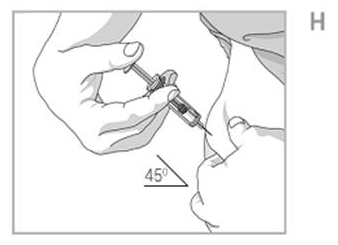
- Using a quick, dart- like motion, insert the needle into the squeezed skin at an angle of about 45degrees. See Figure H.
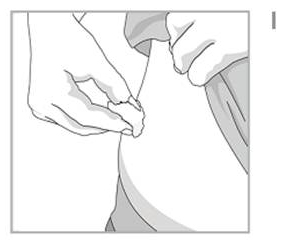
- After the needle is in, let go of the skin. Pull back gently on the plunger.
If blood appears in the syringe:
- It means that you have entered a blood vessel.
- Do not inject Exemptia.
- Pull the needle out of the skin while keeping the syringe at the same angle.
- Press a cotton ball or gauze pad over the injection site and hold it for 10 seconds. See Figure I.
- Do not use the same syringe and needle again. Throw away the needle and syringe in your special sharps container.
- Do not rub the injection site. You may have slight bleeding. This is normal.
- Repeat all the above steps with a new prefilled syringe.
If no blood appears in the syringe:
- Slowly push the plunger all the way in, until all of the liquid is injected and syringe is empty.
- Pull the needle out of the skin while keeping the syringe at the same angle.
- Remove the syringe from the injection site keeping your thumb on the plunger rod.
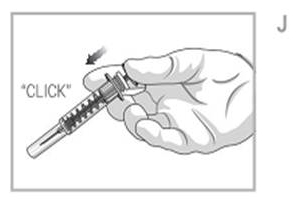
- Orienting the needle away from you and others, activate “Preventis” syringe by firmly pushing the plunger rod. The protective sleeve will automatically cover the needle and an audible “click” will be heard to confirm shield activation. Immediately dispose off the syringe in the nearest sharps collector.
- Press a cotton ball or gauze pad over the injection site for 10 seconds. Do not rub the injection site. You may have slight bleeding. This is normal.
Keep a record of dates and location of your injection sites. To help you remember when to take Exemptia (adalimumab), you can mark your calendar ahead of time.
Proper Storage
How should I store Exemptia?
- Store Exemptia in a refrigerator at 36°F to 46°F (2°C to 8°C) in the original container until it is used. Protect from light.
- When travelling, Exemptia should be stored in a cool carrier with an ice pack.
- Do not freeze Exemptia. Do not use Exemptia if frozen, even if it has been thawed.
- Refrigerated Exemptia may be used until the expiration date printed on the Exemptia(adalimumab) carton and prefilled syringe.
- Do not use the prefilled syringe if the liquid is cloudy, discolored or has flakes or particles in it.
- Keep Exemptia, injection supplies and all other medicines out of the reach of children.
Exemptia Care – Patient Support Programme
We would be happy to help you find the relevant tools and resources to help you in your Exemptia treatment
Patients and their care givers can enrol in our patient care services to avail our services or get responses to their queries:- Email us at exemptiacare@gmail.com
- Call us at 1800-123-CARE (1800-123-2273) from Monday to Friday 10 AM – 6 PM IST (Indian Standard Time)
How to set medication reminders
We know that you are very busy and remembering when to take your Exemptia (adalimumab) medication isn’t always easy. Exemptia CARE offers medication reminders the way that’s most convenient for you. Messages arrive on one day prior to the date you specify for taking the next dosage of Exemptia (adalimumab) and a call comes one day after the date on which you have set up the medication reminder. Plus, you can change your reminder settings at any time by calling. It’s at no additional cost to you.
Set Up Medication Reminders Now
- Calling us at Exemptia CARE toll free number: 1800-123-CARE (1800-123-2273)
- E-mail us at: exemptiacare@gmail.com
FAQs
Fast facts
- Medicines for rheumatoid arthritis (RA) can slow down the disease and reduce damage to joints. They can relieve pain and make it easier to do everyday tasks.
- Most people can find an RA drug that works.
- If one RA drug isn’t working well enough, you have other options. Switching to a different RA drug or adding another kind of RA drug can help.
- Steroids are often used along with other RA drugs. They help with joint pain and swelling. But using them for a long time can cause side effects.
- RA drugs can increase the chance of infections and other side effects. Regular checkups and blood tests are ways to catch these problems early.
Some commonly asked questions
I’ve had RA for several years now. Recently I’ve noticed that whenever I have a flare, my joints creak and crack. It’s loud and sometimes embarrassing, but I’m not in any more pain than usual. Should I be concerned?
The cracking sound is related to the rapid shift of fluid within the joint from one space to another and also to changes within the joint cartilage. During flares, the amount of fluid in the joint space increases; as you move, the snapping of irregular, inflamed tissues can create those cracking and popping sounds. Although it can be annoying, it’s not something to worry about. The best way to put a lid on the noise is to continue to keep RA under control with medication and lifestyle changes.
Is rheumatoid arthritis same as osteoarthritis?
NO. Rheumatoid arthritis is an autoimmune disease, which means your body attacks itself. The target is the synovium, the soft lining around the joints. The immune system sees the synovium as a threat similar to a virus or bacteria and attacks. As a result, fluid accumulates around the joints. The fluid build up causes pain, stiffness, tenderness and inflammatory symptoms of RA. Osteoarthritis, the most common form of arthritis, is a degenerative joint disease. People with OA experience a breakdown of the cartilage that cushions the joints. The wearing down of cartilage causes your bones to rub against each other, which accounts for pain and inflammation. Osteoarthritis does not involve the immune system as in the case of RA.
Does weather affect arthritis pain?
If you have arthritis, you may be among those people (and there are many) who feel that their arthritis pain is influenced by the weather specifically, that they experience more arthritis pain on cold, rainy days and less arthritis pain on warm, dry days. But research studies on whether climate really does affect arthritis pain have produced conflicting results.
How to avoid a rheumatoid arthritis flare?
One of the hardest things about having RA is that you never know when symptoms will flare up. If you’ve gone a long time without one, it can come as a shock. During flares, some people feel frustrated and wonder if they did something wrong. So, let’s clear the air at the start. No one can predict when and why flares occur. It’s not your fault. The best way to keep flares at bay is to take your RA medications consistently. But there are some things you can do to reduce the odds of a flare.
Are you pacing yourself?
On days when you are feeling good, you may be tempted to catch up on all the things you haven’t been able to get done. But be careful not to overdo it. Overdoing activities can bring on fatigue and trigger a flare. On good days, prioritize what needs to be done and pace yourself. Take frequent rest breaks even if you aren’t feeling particularly tired. Ask for help.
Do you protect your joints carefully?
Overusing a joint can trigger painful symptoms and cause more damage. You can help protect your joints in a few key ways.
- Maintain a healthy weight (lose a few pounds if you need to).
- Take advantage of adaptive devices like canes, special jar openers, and padded handles.
- Use good body mechanics — use your largest joints when you lift, carry, or bend.
- Wear safety gear like knee and elbow pads or wrist guards when you play sports or do outdoor activities.
- Move your joints through their full range of motion. Use slow, gentle movements. And do specific exercises to strengthen the muscles and ligaments around your joints. You might ask your doctor for a referral to a physical therapist to get some help learning how to do this.
Do you take your medications on schedule?
It’s so easy to forget, and yet taking your RA medications at the same time every day is the most important thing you can do to prevent a flare. A regular schedule helps you keep a constant, effective level of medication in your blood. Skipping doses can trigger a flare. So use a pill box, a calendar, or an alarm to help keep you on track. If, despite everything, you feel a flare coming on, call your doctor right away. Your doctor may be able to tweak your medications to help keep RA symptoms during the flare under better control.
Is there a cure for rheumatoid arthritis ?
NO, there is no cure for RA, but new effective drugs are increasingly available to treat the disease and prevent deformed joints. In addition to medications and surgery, good self-management, including exercise, are known to reduce pain and disability.
Can i get pregnant if i have rheumatoid arthritis?
Experts disagree whether rheumatoid arthritis affects fertility, but it’s been proven that women with RA do take longer to conceive. This could be chalked up to the side effects of the disease for women, such as low sex drive, inconsistent ovulation, fatigue, and pain. One thing to be aware of is that the medications you might be on for RA may cause birth defects, so you have to work with your doctor to monitor medication if you’re trying to conceive. The minute you and your partner are ready to start trying for baby, see a rheumatologist. Some medications take a month to two years to wash out of your system before it’s safe to conceive. (By the way, that goes for both men and women being treated for RA.) Your rheumatologist will also work out a treatment plan for you while you’re pregnant. Some patients quit medication. Although some women with RA run a slight risk of miscarriage or giving birth to a low-weight baby, the majority of them have normal births without complications. Ironically, 70 to 80 percent of women claim that RA symptoms improved during pregnancy. Another thing to know is that you can’t pass on the disease to your fetus. Though RA has a small genetic component, it doesn’t damage the fetus nor does the baby inherit the disease.
Do RA symptoms improve during pregnancy ?
YES. Research suggests that RA symptoms improve during pregnancy, but symptoms usually return and flares can occur after the baby is born. If you have been diagnosed with RA and you are pregnant or plan to be pregnant soon, talk to your doctor about your medications. Some RA medications are not considered safe during pregnancy, and you may temporarily have to stop taking them. Some medications can also affect fertility in both men and women. Ask your doctor which medications are safe to take when breastfeeding.
Is there a link between rheumatoid arthritis and heart attack ?
People with rheumatoid arthritis have a slightly greater chance of having a heart attack or stroke. The risk is probably reduced by controlling the disease, for example with drug treatments. High cholesterol and smoking increase the risk, so it’s a very good idea to eat a balanced diet and stop smoking.
Do i need any surgery ?
Surgical treatment for rheumatoid arthritis is used to relieve severe pain and improve function of severely deformed joints that don’t respond to medicine and physical therapy. Total joint replacement (arthroplasty) can be done for many different joints in the body. Its success varies depending on which joint is replaced.
Surgeries considered for people who have severe rheumatoid arthritis include:
- Arthroplasty, to replace part or all of a joint, such as the hip or knee.
- Arthroscopy, which uses a small lighted instrument to remove debris or inflamed tissuefrom a joint.
- Carpal tunnel release, to relieve pressure on the median nerve in the wrist.
- Cervical spinal fusion, to treat severe neck pain and nerve problems.
- Finger and hand surgeries, to correct joint problems in the hand.
- Foot surgery such as phalangeal head resection.
- Synovectomy, to remove inflamed joint tissue.
Joint surgery often restores near-normal movement in a person who has osteoarthritis in just one or two joints. But this is not the case for people affected by rheumatoid arthritis.
I have rheumatoid arthritis (RA) and whenever I have a particularly bad flare, my voice becomes very raspy. Sometimes my throat is so swollen that I actually lose my voice. Could my RA be the blame?
Hoarseness can indeed be related to your RA. Although many people aren’t aware of it, the throat contains cartilage that can become inflamed during a flare. The swelling can affect your voice and even impair your breathing. Mention this symptom to your rheumatologist, and in the meantime, stay clear of smoky areas and try not to strain your voice.
Can uv rays ease ra pain?
There is no evidence whatsoever that tanning beds have a favorable effect on RA symptoms. In fact, depending on what medications you’re taking, your condition may actually be worsened when you’re exposed to UV rays. Besides, certain RA medications may increase the risk of skin cancer.
What is a good healthy diat to follow?
It is important to follow a healthy, balanced diet that includes:
- Whole grains, like oatmeal or brown rice
- Fruits and vegetables
- Low or no saturated fat, especially animal fat
- Low amounts of salt and sugar
- The daily recommended amount of vitamins and minerals
Research has also suggested that eating foods rich in omega-3 fatty acids, such as fish, can help reduce inflammation in your body. If you drink alcohol, do so in moderation. If you notice certain foods seem to increase the swelling in your joints, try to avoid them. Maintaining emotional health: You can also improve your physical health by improving your emotional health. High levels of stress might increase your tendency to experience flares and might make it more difficult to deal with the challenges of living with RA.
You can take steps to understand and control your stress:
- Spend some time to identify what stresses you by keeping a journal or diary.
- Try to avoid things that contribute to your stress.
- Develop positive ways to cope, like making time for hobbies you enjoy or simply relaxing in a quiet space each day.
Sometimes, you might find yourself feeling frustrated or sad about some of the challenges you face when living with RA. Tasks that used to be simple might now be difficult or might require the help of others. Some days, pain and fatigue might leave you feeling helpless or overwhelmed. It’snormal to feel this way, especially at first. It can help to seek support from friends and family ortake extra time to do things that make you happy. You might want to find a support group or online message board for people with RA.
Protecting your bones
Together with your doctor, you will want to track the health of your bones. You may want to ask your doctor whether you should take a bone density test. Many people with RA develop osteoporosis, a condition in which the bones become brittle and easy to break. This is especially true if you take large doses of corticosteroids, such as prednisone, over a long period of time. There are several steps you can take to help prevent osteoporosis:
- Get enough calcium and vitamin D in your diet.
- Do gentle, weight-bearing exercise, like walking, as recommended by your doctor.
- Do not smoke.

